Clinical Documentation Improvement (CDI) – The shift to Outpatient and Quality: Where can CDI and Coding make an impact?
Over the last several years there has been a steady shift in focus from traditional inpatient clinical documentation improvement (CDI) programs towards outpatient CDI and Quality Improvement programs. This shift is largely due to the maturation of longstanding inpatient DRG focused programs seeking additional revenue streams and the phasing in of government sponsored programs such as Value Based Purchasing (VBP). Quality and Outpatient metrics are largely driven by factors outside the scope and responsibility of CDI and coding (e.g., patient satisfaction surveys).
Where CDI specialists and coders can make the most impact on Quality and Outpatient metrics is by ensuring that the severity of illness (SOI) levels are accurately reported and appropriate Hierarchical Condition Categories (HCCs) are captured. Outpatient audits often utilize the inpatient record to verify diagnoses reported in the outpatient setting which is why it is critical that all clinically significant diagnoses are clearly and accurately documented and coded. Below are examples of diagnoses and their impact on HCCs and SOI scores compared to MS-DRG impact:
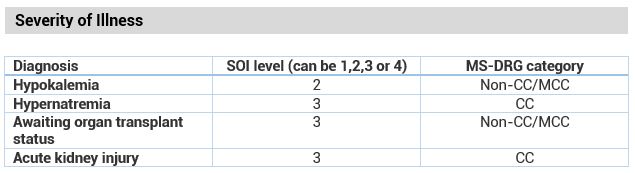
- Electrolyte abnormalities such as hypokalemia impact the SOI score even though they do not impact the MS-DRG
- Awaiting organ transplant significantly impacts the SOI score but does not impact the MS-DRG
- Some conditions such as AKI impact both the SOI and MS-DRG assignment
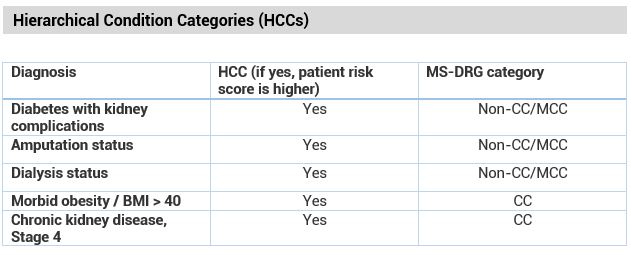
- Most MS-DRG CC/MCCs are also HCCs
- Even though “status codes” do not impact MS-DRGs, they do significantly impact the HCC risk adjustment score and should always be reported
As CDI programs continue to expand it is critical that CDI specialists and coders stay up to date with how documentation and ICD-10 codes are being utilized outside the inpatient setting. Understanding the SOI scoring system and HCCs can help ensure critical patient data is being captured accurately in all settings. Being fluent in multiple payment/data capture methodologies will ensure that coders and clinical documentation specialists stay relevant in the ever-changing landscape of healthcare reimbursement and quality tracking.
