Recently, the Centers for Medicare and Medicaid Services (“CMS”) released data showing that all but one state has seen the Medicare 30-day readmission rates fall due to the Hospital Readmission Reduction Program (“the Program”). The readmission rate fell by more than 5% in 43 states and by more than 10% in 11 states. See the chart below released by CMS:
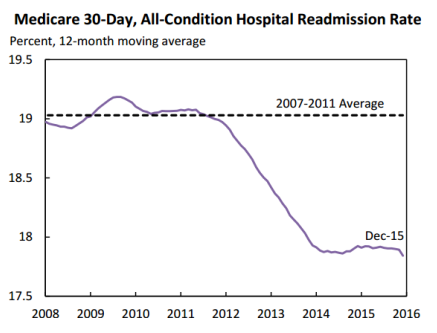
CMS also stated that “Medicare beneficiaries avoided almost 104,00 readmissions in 2015 alone” when compared to the 2010 levels. In all, the Health and Human Services Assistant Secretary of Planning and Evaluation estimates that since 2010, Medicare beneficiaries have avoided 565,000 readmissions.
The Hospital Readmission Reduction Program was established by the Affordable Care Act. The Program allows for CMS to adjust payment for hospitals with higher than expected 30-day readmission for targeted clinical conditions that include heart attacks, heart failure and pneumonia. CMS also credits other major quality improvement initiatives, like the Partnership for Patients, for the reduction in the readmission rates.
